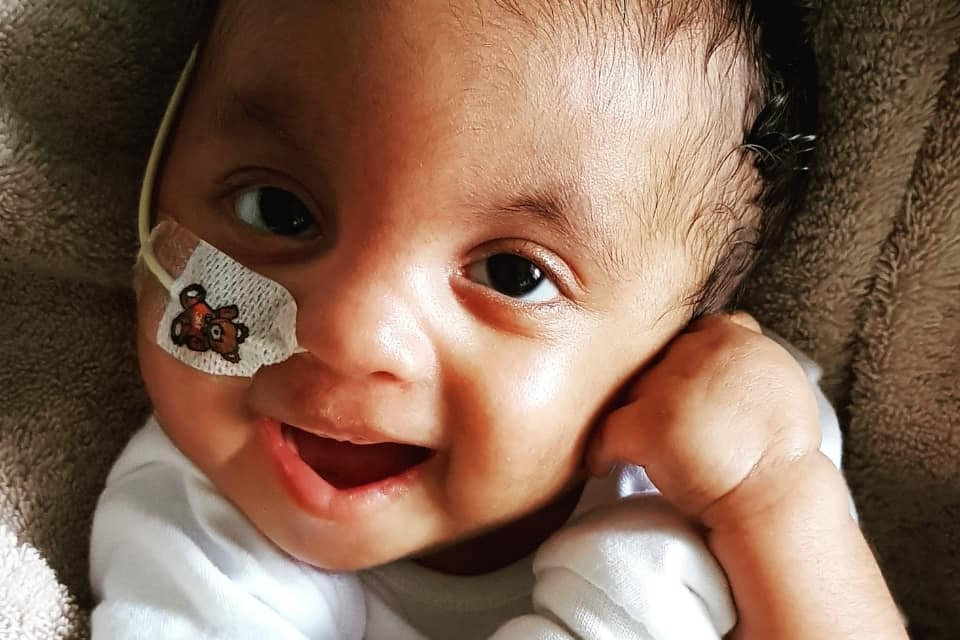
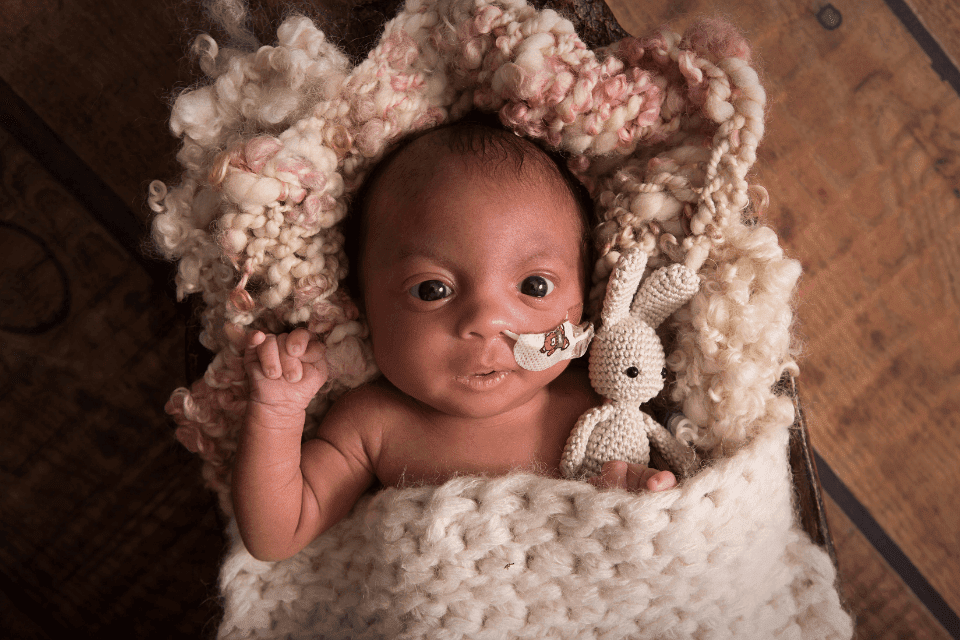
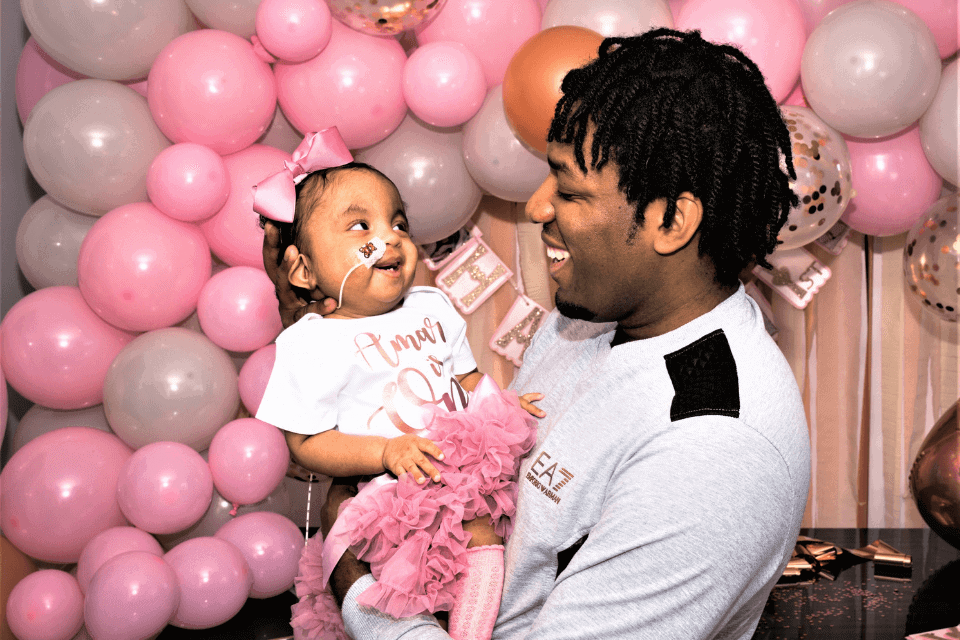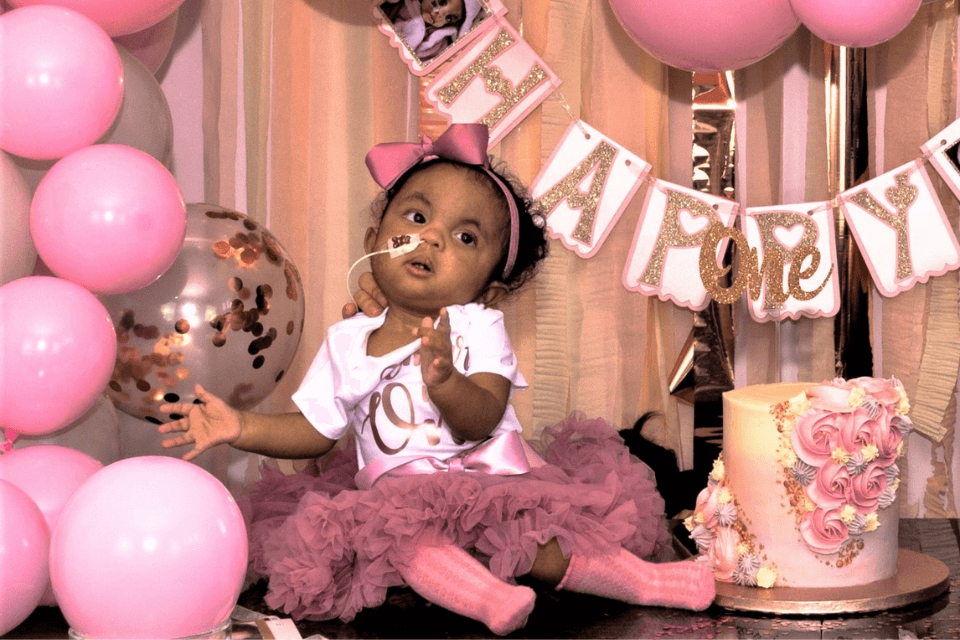Amanda says: “Amari lives with clenched fists, rocker bottom feet, a hole in her heart, cysts on the brain, delayed mental development, small stature, chronic constipation controlled by a daily dose of laxatives, oral feeding problems that mean she’s fed via a tube, poor muscle strength meaning she cannot yet sit up or crawl, semi-frequent spasms and a flat side to her skull caused by tight neck muscles.
“Amari is her own person, though, and we’ve known that ever since we saw her striking yoga poses and giving us a wave at ultrasound scans during pregnancy. Today she smiles, laughs, anticipates, wonders, plays, moans when she doesn’t want to do something, has diva moments and, of course, just gives out an abundance of unconditional love!”
Amanda never imagined being able to describe Amari’s character in such a way after being told her daughter was at high risk of Edwards’ syndrome during her 12-week scan.
“This was the worst and most unexpected news I’ve ever had in my life, and was undoubtedly the worst part of my journey with Amari to date. Unfortunately, due to the current statistics around trisomy 18, the medical profession tell every person deemed as having a high-risk pregnancy in this respect that their baby is ‘incompatible with life’, then proceed to list all the health issues the baby could have and suggest they’ll most likely live a life full of suffering. You are then asked if you’d like to terminate the pregnancy. There are no positive stories shared at this point, so you feel completely devastated and alone.
“In a nutshell, my world was shattered. I cried, I felt it was so unfair this should happen to me and my husband, especially after we struggled to conceive for around four years before I eventually fell pregnant with Amari. The rate of babies diagnosed with trisomy 18 is one in 2,500 pregnancies, so it felt especially cruel at the time. There is just nothing that can prepare you for the loss of the future you thought you’d have with your child and that you took for granted as being a given. It is a struggle I still deal with today, although on a much lesser scale as I appreciate each and every day we get with Amari.”
One source of support for Amanda and the family has been East Anglia’s Children’s Hospices (EACH). Initially, during Amari’s first six months, they were supported by EACH’s Symptom Management Nursing Service. The specialist support was such that Amanda says it was a “bittersweet time” when they realised Amari had improved to the point of no longer requiring it.
She explains: “We knew it was a good thing for Amari to be taken off ‘end of life’ support, but we’d built some lovely relationships with the team we were really going to miss.”
EACH’s support for the family started when Amari was born in hospital, with a member of our care team joining them to help make memories and keepsakes, including hand and foot casts, and hand and foot prints on canvas.
Amanda says: “EACH being at the hospital helping us to make memories when we thought we may not have met Amari alive, or we’d only have a few hours or days with her, was something we’ll appreciate forever, even though we’ve been blessed with much more time with Amari than we thought we’d have.
“We were also visited by other members of the EACH team to talk about whether we’d like to take Amari home and be supported with end of life care, or whether we’d like to take her to EACH’s hospice in Milton to be supported there. We decided to take her home with us after two days in the hospital and two bouts of apnoea in which she didn’t breathe for what seemed like forever, and turned blue, but slowly recovered after taking a breath. We thought if she was going to pass away suddenly in that way then we’d rather take her home and enjoy whatever time we had with her where she was always intended to be. The EACH team fully supported our decision and followed us home from the hospital, providing a big box of ‘just in case’ drugs so that Amari could have strong pain relief, if anything happened, and pass peacefully, our main priority at the time. They explained how to use the drugs, what to expect to see and experience if Amari did pass away, and alerted us to the availability of their emergency hotline so that we didn’t have to feel alone if anything happened. Their support was so vital to us during those early days as we were scared and uncertain of what was ahead of us.
“Over the passing days and weeks, we had weekly house visits from the EACH team to check on Amari’s condition. They would check her heart rate, breathing, skin colour, hydration, eyes, everything. They noted everything down and kept us up to date with her progress from a medical/end of life standpoint. Again, those visits were so invaluable to us as they gave us some kind of indication as to how well or badly Amari was doing, allowing us to prepare for the next day ahead of us. That is how we managed, just one day at a time.
“When Amari continued to show signs of getting healthier, after we switched to nasogastric tube feeding to get her to put on weight, we agreed visits from EACH would be every three weeks, then after further improvement we agreed we could arrange house visits only if Damian and I decided it was necessary.
“Just knowing EACH is still there and willing to help and support us is another important comfort. This journey is difficult and uncertain, and what EACH provides is some form of certainty in the guidance and support they provide to families facing the loss of a child.”
Amanda credits being able to completely enjoy time with Amari, rather than worry about what lies ahead, to the experience of EACH staff.
“EACH were the ones to tell us we could stop living with the expectation Amari was going to die imminently, due to how well she was doing on each visit. They told us to, instead, enjoy our time with her and make memories rather than focus on the negatives. It sounds silly because although we had this same aim in our minds we were trying to stay grounded and brace ourselves for the imminent and certain death of our child, so it took that small suggestion from people with experience to allow us to adjust our mindset and stop living with fear as the predominant emotion. For me, it allowed me to open my heart up to loving Amari fully as I’d been trying to hold back becoming attached in preparation for dealing with the inevitable grief that was to come.”
Another aspect of EACH’s service Amari has been able to benefit from is hydrotherapy. She had a first session at Milton just before the pandemic struck.
Amanda recalls: “I’ll always treasure the memory of getting our two-month-old Amari in her oversized yet still tiny swimming costume into the warm hydrotherapy pool, with the lovely team at the hospice. Amari was just so at ease in the pool and yawning so much in the water as she was so relaxed. It was so lovely to have that bonding time with her and to be showed all the different exercises by the team. Amari is definitely a water baby by nature! We look forward to enjoying those sessions again after the pandemic.”
Families’ stories and experiences are unique to them and we have been kindly granted permission to share this family’s story. If you have been affected by what you’ve read or have a question and would like to talk to someone, please contact your local children’s hospice service or Together for Short Lives, the UK charity that supports families caring for seriously ill children (tel: 0808 8088 100).
Would you like us to write and share your own family story?
We give all those receiving support from EACH the opportunity to share their family story. All family members are welcome to get involved if they’d like to and we will never share your story until you are completely happy with it. If you have any questions or are interested in finding out more, please contact Matt Plummer, EACH Media and PR Manager at matt.plummer@each.org.uk.